Special Education and Needs Resources

Get Help Teaching Special Needs Students
From the basics to inclusion and behavior management, select a category of special education resources below.Special Education Resources By Topic
Accommodations and Environment Curriculum Support IEP Resources Behavior Management Special Education Inclusion
Understanding that special education resources are applicable to both general education and special education teachers alike, TeacherVision provides resources that can be used as part of an IEP both in the general education classroom and in specialist resources rooms. Our resources have been curated from leading special education partners and publishers, and are easily categorized for the most common uses by both generalists and specialists.
What Is Special Education?
Special education can generally be defined as the integration of instructional, behavioral, social-emotional, developmental, and curricular support services and strategies designed to help students with disabilities learn. Special education resources and services are usually delivered across a variety of school settings, depending on the needs of the child and the availability of school staff and environment.
Some special education students may spend part of their time in an integrated classroom, receiving instruction from generalists and interacting with classmates, with scheduled interventions from specialists (speech, language, behavioral, physical therapy, etc.). Others may spend the bulk of their time in dedicated special services environments, with specialized physical, developmental, and learning supports.
Most students designated for special education services will receive an Individualized Education Program (IEP). IEP special education services take into account the varying needs among special education students, and tailor learning and specialized services for each individual student. In most cases, an IEP special education plan involves the development and implementation of specific accommodations designed to meet the needs of each individual student, both in the general education classroom and in specialist resource rooms.
Accommodations and Environment
These special education classroom resources have been specially selected to help general and special education teachers with instructional and environmental accommodations and supports, such as assessment accommodation, special education classroom setup, accommodations for disabilities, and more.
Curriculum Support
These resources provide generalists and special education teachers with strategies and tools for developing and implementing special education curriculum supports. Included are special education lesson plans, special education activities, and other materials for academic instruction and support.
Behavior Management
Use these special education behavior management resources to plan and implement behavior management strategies in integrated and special education classrooms.
IEP Resources
This collection of IEP special education resources gives general education teachers, special education teachers, and parents all the IEP forms, accommodations, strategies, and advice necessary for planning and implementing an Individualized Education Plan in both the general ed classroom and specialist resource rooms.
Special Education Inclusion
Various techniques, tips, and suggestions for promoting special education inclusion in integrated general education classrooms are included in these resources, such as, using stories about children with disabilities to teach others, and proactive tips and effective techniques in your classroom.
Recommended Special Education and Needs Resources Resources
-
TEACHING RESOURCE
Teaching Students with Special Needs
Download for free! Prepare to teach students with special needs in your classroom using these effective strategies to ... -

TEACHING RESOURCE
Positive Descriptions of Student Behavior
-

TEACHING RESOURCE
What Is Comprehensible Input for ELL Students?
10 tips and strategies to help English-language learners thrive in your classroom. English-language learners often stru... -

TEACHING RESOURCE
Using Multiple Intelligences in Testing & Assessment
Download for free! Information on using Howard Gardner's theory of multiple intelligences (MI) in student assessments i... -

TEACHING RESOURCE
Collaboration Between General and Special Education Teachers
Communication and collaboration between general and special education teachers is vital to the success of special needs ... -

WORKSHEETS
Effective Accommodations for Students with IEPs
A complete chart to help IEP teams find specific accommodations in instruction, assessment, classroom management, organi... -
TEACHING RESOURCE
Scope of the Mathematics Curriculum
This professional development resource will help you discover the process and content standards for teaching a successfu... -
REFERENCE
Teaching Mathematics to Gifted Students in a Mixed-Ability Classroom
-
TEACHING RESOURCE
Communicating with Culturally Diverse Parents of Exceptional Children
-
TEACHING RESOURCE
The IEP Cycle: The General Educator's Role
-
REFERENCE
Frequently Asked Questions on Inclusion
-
TEACHING RESOURCE
Modifying Instruction: Teaching Students with ADD
Suggested modifications to make for students with ADD/ADHD, including lesson presentation, physical arrangement of the c... -
TEACHING RESOURCE
Adapting Language Arts, Social Studies, and Science for the Inclusive Classroom
-

TEACHING RESOURCE
How to Manage Disruptive Behavior in Inclusive Classrooms
Effective behavior management for inclusive classrooms Managing disruptive behavior is examined in detail. The teaching... -
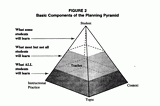
WORKSHEETS
Structuring Lessons for Diverse Learners -- Planning Pyramid
The Planning Pyramid is a framework for planning for diverse student needs and assists in differentiating instruction in... -
TEACHING RESOURCE
Introduction to Portfolios
Improve outcomes with this impactful assessment strategy Learn how to design and implement a portfolio assessment progr... -

TEACHING RESOURCE
Proactive Measures for Behavior Management
-

TEACHING RESOURCE
Keys to Successful Inclusion
-

WORKSHEETS
Accommodations Checklist
-
TEACHING RESOURCE
Six Principles of Effective Curriculum Design for Inclusive Classrooms
Special educators show how to design and deliver lessons that are truly inclusive Developing lesson plans and curriculu... -

ACTIVITIES
Repeated Reading
-
TEACHING RESOURCE
Collaboration in Today's Math Classroom
Today's math teachers must provide high-quality instruction to very diverse students. All teachers responsible for mathe... -
TEACHING RESOURCE
Planning Pyramid for Multi-Level Mathematics Instruction
-

TEACHING RESOURCE
Direct Skill Instruction for Students with Autism
This article identifies social skills that need to be developed with autistic students and the steps required to build t...








